Dental Implant Post-Op Instructions: A Comprehensive Guide
Dental implants offer a lasting solution for missing teeth, mirroring natural tooth function and appearance. The entire process, from consultation to final restoration,
typically spans three to six months, with healing being a crucial component. Successful osseointegration, where the implant fuses with the jawbone, is essential for long-term stability.
Initial 24-48 Hours: Immediate Post-Operative Care
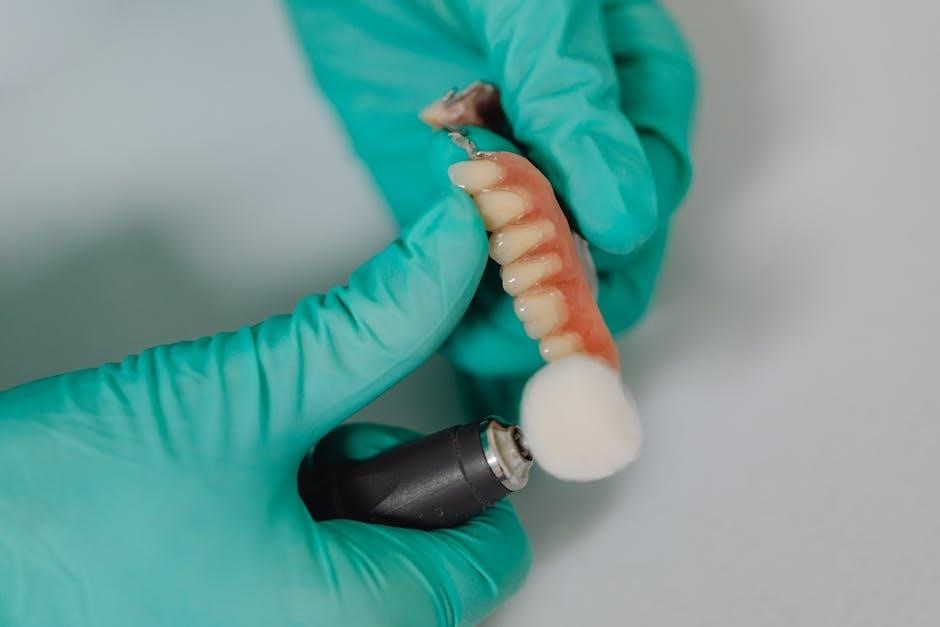
The first 24-48 hours following your dental implant surgery are critical for initiating the healing process. You’ll likely feel groggy from the anesthesia, so rest is paramount. Avoid strenuous activity, as it can increase bleeding and swelling. Directly after surgery, apply firm, consistent pressure to the surgical site using gauze pads provided by your dentist; change these pads every 30-45 minutes, or as directed, until bleeding subsides.
Expect some minor bleeding and oozing – this is normal. If excessive bleeding occurs, apply continuous pressure for a longer duration. Avoid disturbing the surgical site by touching it with your tongue or fingers. Stick to a liquid diet during this period, avoiding hot or carbonated beverages.
Medication, as prescribed by your dentist, should be taken as directed, including pain relievers and antibiotics. Keep your head elevated, even while sleeping, to minimize swelling. Gentle oral hygiene, such as rinsing with a saltwater solution (warm water with ½ teaspoon of salt), can begin 24 hours post-surgery, but avoid vigorous rinsing or spitting.
Managing Pain and Discomfort
Post-operative pain and discomfort are common after dental implant surgery, but manageable. Your dentist will likely prescribe pain medication – take it as directed, even if you aren’t experiencing significant pain, to stay ahead of discomfort. Over-the-counter pain relievers, like ibuprofen or acetaminophen, may also be recommended or used in conjunction with prescription medication, always following your dentist’s guidance.
Ice packs applied to the outside of your cheek in 20-minute intervals (20 minutes on, 20 minutes off) during the first 24-48 hours can significantly reduce swelling and numb the area, alleviating pain. Rest is crucial; avoid strenuous activities that can exacerbate discomfort.
A soft food diet is essential during the initial healing phase, minimizing chewing and pressure on the surgical site. Ensure you are well-hydrated; If pain persists or worsens despite medication, contact your dentist immediately. Remember, some mild discomfort is expected, but severe or escalating pain could indicate a complication requiring attention.
Bleeding Control Techniques
Some bleeding is normal following dental implant surgery. Immediately after the procedure, your dentist will likely have you bite down firmly on gauze pads. Maintain consistent pressure by replacing these pads every 30-60 minutes, or as directed, until the bleeding subsides. Avoid spitting, as this can disrupt clot formation and prolong bleeding.
Rest is paramount. Elevate your head with pillows to minimize blood flow to the surgical area. Avoid strenuous activity for at least 24-48 hours, as this can increase bleeding. Do not rinse vigorously; gentle rinsing with saltwater (after 24 hours, as advised by your dentist) is permissible, but forceful swishing should be avoided.

If bleeding continues excessively or doesn’t diminish after several hours, contact your dentist. A moistened tea bag (black tea contains tannic acid, which aids clotting) can be gently applied to the site if gauze isn’t sufficient, but consult your dentist first. Avoid disturbing the surgical site with your tongue or fingers.

Swelling Management: Ice Packs and Elevation
Post-operative swelling is a common occurrence after dental implant surgery. Applying ice packs to the outside of your cheek in the area of the implant is highly recommended. Use the ice packs for 20 minutes on, and 20 minutes off, during the first 48-72 hours. Never apply ice directly to the skin; always use a cloth barrier to prevent skin damage.
Elevating your head, even while resting, significantly aids in reducing swelling. Prop yourself up with pillows to keep your head higher than your heart. This helps to minimize blood flow to the surgical site, lessening inflammation. Avoid bending over or engaging in strenuous activities that could increase blood pressure.
While ice is most effective in the initial days, after 72 hours, warm compresses can be used to promote blood flow and aid in the healing process. Continue to rest and follow your dentist’s instructions carefully. Managing swelling is crucial for comfort and optimal recovery.
First Week: Early Healing Phase
The first week following dental implant surgery is critical for initial healing. Expect some discomfort, bruising, and swelling – these are normal responses to the procedure. Focus on rest and adhering strictly to your dentist’s post-operative instructions. Avoid strenuous activity, as it can increase bleeding and swelling.
Dietary restrictions are paramount during this phase. Stick to soft foods like yogurt, applesauce, and mashed potatoes. Avoid chewing on the side of your mouth where the implant was placed. Hydration is also essential; drink plenty of fluids, but avoid using straws, as the sucking motion can disrupt clot formation.
Gentle oral hygiene is vital. Continue to brush and floss, but be extremely careful around the surgical site. Your dentist may recommend a special mouthwash to keep the area clean and prevent infection. Most patients experience significant recovery within the first two weeks, but continued care is essential.
Dietary Restrictions: Soft Food Choices
Following dental implant surgery, adhering to dietary restrictions is crucial for successful healing. During the initial recovery period, prioritize soft foods that require minimal chewing. This protects the surgical site and promotes optimal osseointegration; Avoid hard, crunchy, or chewy foods that could damage the implant or surrounding tissues.
Excellent soft food choices include yogurt, applesauce, mashed potatoes, smoothies, soups (lukewarm, not hot), scrambled eggs, and well-cooked pasta. Gradually introduce slightly more textured foods as your comfort level increases. Continue to avoid foods that are spicy, acidic, or contain small particles that could become lodged in the surgical area.
For the first week, chew primarily on the side of your mouth opposite the implant site. Even after a week, continue to avoid tough or crunchy foods on the implant side. Remember, a patient is usually fully recovered after two weeks, but careful eating habits are vital during the early stages of healing.
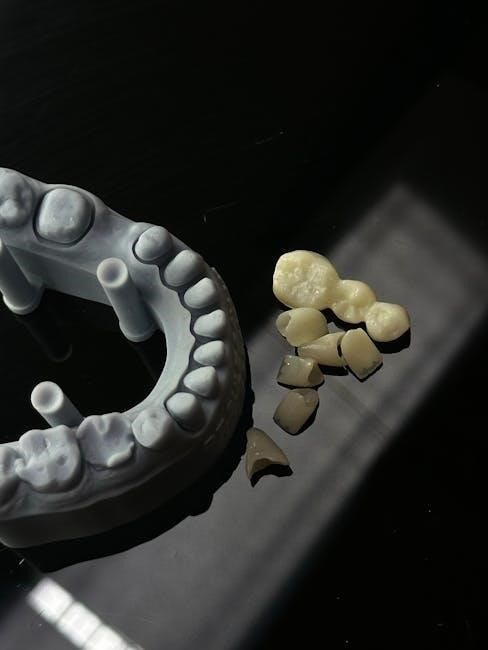
Oral Hygiene: Gentle Cleaning Practices
Maintaining meticulous oral hygiene is paramount after dental implant surgery, but it requires a gentle approach. Avoid vigorous brushing or rinsing that could disrupt the healing process. Initially, rinse your mouth gently with saltwater several times a day, especially after meals, to keep the area clean and promote healing.
Use a soft-bristled toothbrush to carefully clean the surrounding teeth and gums, avoiding direct contact with the implant site for the first few days. Your dentist may recommend a special antimicrobial mouthwash to further reduce bacteria. Continue this gentle cleaning routine throughout the early healing phase.
As healing progresses, you can gradually resume your regular brushing and flossing habits, but always be mindful of the implant site. Proper oral hygiene is essential not only for preventing infection but also for ensuring long-term implant success and avoiding late complications.
Medication Management: Pain Relievers & Antibiotics
Following your dental implant surgery, your dentist will likely prescribe pain relievers and antibiotics to manage discomfort and prevent infection. Take all medications exactly as prescribed, completing the full course of antibiotics even if you feel better. Do not exceed the recommended dosage of pain relievers.
Over-the-counter pain relievers, such as ibuprofen or acetaminophen, may be sufficient for managing mild discomfort, but consult your dentist before using them in conjunction with prescribed medications. Be sure to inform your dentist of any existing medical conditions or other medications you are taking to avoid potential interactions.
If you experience any adverse reactions to the medications, such as allergic reactions or severe side effects, contact your dentist immediately. Proper medication management is crucial for a smooth recovery and minimizing the risk of complications after your dental implant procedure.
Recognizing and Reporting Complications
While dental implant surgery is generally safe, it’s vital to be aware of potential complications and know when to contact your dentist. Signs of infection, such as increased pain, swelling, redness, pus, or fever, require immediate attention. Report any unusual symptoms promptly; delaying treatment can worsen the issue.
Other complications may include excessive bleeding that doesn’t subside with pressure, numbness or tingling that persists beyond the initial post-operative period, or implant instability. If you experience any loosening of the implant or surrounding teeth, contact your dentist immediately.
Don’t hesitate to report any concerns, even if they seem minor. Early detection and intervention are key to resolving complications effectively and ensuring the long-term success of your dental implant. Your dentist is your best resource for addressing any issues that may arise during the healing process.
Weeks 2-4: Intermediate Healing
During weeks two to four, the initial healing phase transitions into a period of intermediate recovery. You may experience a significant reduction in discomfort and swelling, though some minor sensitivity is normal. Continue to follow your dentist’s instructions diligently to promote optimal healing and osseointegration.
Dietary progression should continue, gradually introducing slightly more textured foods. Avoid hard, crunchy, or chewy items that could put stress on the implant site. Focus on soft, nutritious meals that support tissue repair. Maintaining meticulous oral hygiene is crucial; gently brush and rinse as directed, avoiding the surgical area directly unless specifically instructed.
Continue taking any prescribed medication as directed, even if you feel better. Attend any scheduled follow-up appointments to allow your dentist to monitor your progress and address any concerns. Remember, patience is key during this phase, as the implant continues to integrate with your jawbone.
Gradual Dietary Progression
Following dental implant surgery, a carefully planned dietary progression is vital for successful healing. Initially, stick to a strictly soft food diet – think smoothies, yogurt, applesauce, and mashed potatoes. Avoid chewing directly on the implant site. As the first week passes, you can slowly introduce slightly more textured foods, like soft-cooked pasta, scrambled eggs, and well-moistened fish.
Around two weeks post-op, many patients feel comfortable adding more variety, but continue to avoid hard, crunchy, or chewy foods. These can disrupt the healing process and potentially damage the implant. Continue to chew on the opposite side of your mouth. Gradually reintroduce foods like tender chicken, cooked vegetables, and soft fruits.
Listen to your body and don’t rush the process. If a food causes discomfort, revert to a softer option. Proper nutrition supports tissue regeneration and osseointegration. Remember, a patient is often fully recovered after 2 weeks, but caution is still advised.
Continued Oral Hygiene: Brushing & Rinsing
Maintaining impeccable oral hygiene is paramount after dental implant placement. While gentle, it’s crucial to begin cleaning around the implant site as soon as possible, but with modifications. Use a soft-bristled toothbrush and brush carefully, avoiding direct pressure on the surgical area. Focus on cleaning the surrounding teeth and gums to prevent plaque buildup.
For the first few days, avoid vigorous rinsing. Your dentist may recommend a chlorhexidine mouthwash to help control bacteria, but follow their specific instructions. After the initial healing phase, gently rinse your mouth with warm salt water several times a day. This helps keep the area clean and promotes healing.

As healing progresses, you can gradually return to your regular brushing routine, but continue to be gentle around the implant. Regular dental check-ups and professional cleanings are essential for long-term implant health. Consistent hygiene prevents peri-implantitis, an inflammation around the implant.
Suture Care (If Applicable)
If your dental implant procedure involved sutures (stitches), proper care is vital for optimal healing and to prevent infection. Your dentist will provide specific instructions, but generally, you should keep the area clean and dry. Avoid touching or disturbing the sutures.
Typically, sutures will dissolve on their own within two weeks, but some may need to be removed by your dentist. Do not attempt to remove them yourself. Gently rinse your mouth with warm salt water as directed to keep the area clean and promote healing.
Be vigilant for signs of infection, such as increased pain, redness, swelling, or pus. If you experience any of these symptoms, contact your dentist immediately. Avoid consuming hard, crunchy, or sticky foods that could irritate the suture site or dislodge the stitches. Following your dentist’s suture care instructions diligently will contribute significantly to a successful recovery.
Monitoring for Infection Signs
Post-dental implant surgery, diligently monitoring for infection signs is crucial for a smooth recovery. While some discomfort is normal, be alert for changes that could indicate a problem. Increased pain beyond what your pain medication manages is a key indicator.
Redness and excessive swelling around the implant site, especially if it worsens after the initial few days, should be reported to your dentist. The presence of pus or discharge from the surgical area is a clear sign of infection. A fever of 100.4°F (38°C) or higher is also a concerning symptom.
If you experience any of these signs, contact your dentist immediately. Early detection and treatment of infection are essential to prevent complications that could jeopardize the implant’s success; Remember, proactive monitoring and prompt communication with your dental team are vital for a healthy recovery process.
Months 2-6: Osseointegration & Final Restoration
Months two to six mark the critical osseointegration phase, where the implant fuses with your jawbone. This process, vital for long-term stability, requires patience and adherence to post-operative instructions. While you may feel improved comfort, continued care is paramount.
Follow-up appointments are scheduled to evaluate progress. Your dentist will assess bone density and implant stability, often using imaging techniques. You might experience subtle sensations during this period, which are generally normal as the bone integrates with the titanium.
As osseointegration nears completion, preparation for abutment placement begins. The abutment, a connector piece, will eventually support your final restoration. This stage involves a minor surgical procedure. Finally, your custom-made crown, bridge, or denture is attached, completing the transformation and restoring your smile. Remember, the entire process can take three to six months.
Osseointegration Process Explained
Osseointegration is the cornerstone of dental implant success – the biological process where the implant directly fuses with the living bone. This creates a strong, stable foundation for your replacement tooth. It’s not a quick fix; it requires dedicated healing time, typically three to six months, allowing bone cells to grow onto and into the implant surface.
Initially, a biological response occurs, forming a layer of bone around the implant. Over time, this layer thickens and strengthens, effectively becoming part of the jawbone. Factors influencing osseointegration include implant surface characteristics, bone quality, and overall health.
During this phase, you may experience minor discomfort or sensations, which are generally normal. Strict adherence to post-operative instructions – including a soft diet and meticulous oral hygiene – is crucial. Successful osseointegration ensures the implant can withstand the forces of chewing and provide a long-lasting, functional, and aesthetically pleasing result.
Follow-Up Appointments & Progress Evaluation
Regular follow-up appointments are vital throughout the dental implant process, ensuring optimal healing and long-term success. These visits allow your dentist to meticulously monitor osseointegration and assess the overall health of the implant site. Initial check-ups typically occur within the first few weeks post-surgery, then at intervals of three to six months.
During these appointments, your dentist will evaluate your bite, gum tissue, and the stability of the implant. X-rays are commonly used to visualize bone growth around the implant, confirming successful fusion. Any concerns or discomfort you’re experiencing will be addressed, and adjustments to your treatment plan can be made if necessary.
Progress evaluation isn’t just about physical healing; it also involves assessing your comfort and function. Your dentist will ensure the implant feels natural and doesn’t interfere with your daily activities. Consistent attendance at these appointments is key to identifying and addressing any potential issues early on, safeguarding your investment in a healthy, beautiful smile.
Potential Sensations During Osseointegration
Osseointegration, the process where the implant fuses with your jawbone, isn’t always symptom-free. While generally comfortable, patients may experience a range of sensations during this three to six-month period. It’s common to feel mild discomfort or a dull ache at the implant site, particularly in the initial weeks. This is usually manageable with over-the-counter pain relievers as recommended by your dentist.
Some individuals report a sensation of warmth or tingling around the implant, which indicates healthy bone remodeling. You might also notice slight pressure or sensitivity when chewing, especially if the implant is still adjusting. These sensations are typically temporary and diminish as osseointegration progresses.
However, it’s crucial to differentiate normal sensations from potential complications. Any sharp, persistent pain, excessive swelling, or signs of infection warrant immediate attention. Open communication with your dental team is vital to ensure a smooth and successful healing process.
Abutment Placement Preparation
Once osseointegration is confirmed – typically after three to six months – the next step is preparing for abutment placement. The abutment serves as a connector between the implant and the final restoration, like a crown. This usually involves a minor surgical procedure performed under local anesthesia.
Before the procedure, your dentist will assess the implant site to ensure adequate healing and stability. They may take new impressions of your mouth to create a precisely fitted abutment. It’s important to maintain excellent oral hygiene during this phase to minimize the risk of infection.
You’ll receive specific instructions regarding pre-operative preparations, which may include adjusting any medications you’re taking. Following these guidelines carefully will contribute to a successful abutment placement and pave the way for your permanent tooth restoration. Remember to discuss any concerns or questions with your dental team beforehand.
Long-Term Implant Care
Dental implants, while durable, require consistent long-term care to ensure their longevity and functionality. Maintaining optimal oral hygiene is paramount. This includes brushing twice daily with a soft-bristled toothbrush, flossing daily, and using an antimicrobial mouthwash as recommended by your dentist.
Regular dental check-ups and professional cleanings are crucial – typically every six months – to monitor the implant’s stability and address any potential issues early on. Your dentist will assess the surrounding tissues and ensure there are no signs of peri-implantitis, an inflammatory condition affecting the tissues around the implant.
Avoiding habits that can damage implants, such as smoking, excessive alcohol consumption, and using teeth as tools, is vital. Be mindful of parafunctional habits like teeth grinding or clenching, and discuss solutions with your dentist if necessary. With diligent care, your dental implant can provide years of confident smiles and reliable function.
Maintaining Optimal Oral Hygiene
Optimal oral hygiene is the cornerstone of long-term implant success. Begin with a soft-bristled toothbrush, gently cleaning around the implant and gum line twice daily. Avoid abrasive toothpastes, as they can scratch the implant surface. Flossing is equally important, removing plaque and food particles from between teeth and around the implant.
Consider using interdental brushes or water flossers to reach areas a standard toothbrush and floss might miss. An antimicrobial mouthwash, recommended by your dentist, can further reduce bacteria and maintain a healthy oral environment. Pay close attention to cleaning along the gumline, as this is where inflammation often begins.
Regularly inspect your gums for signs of redness, swelling, or bleeding. Promptly address any concerns with your dental professional. Consistent, gentle, and thorough oral hygiene practices are essential for preventing complications and ensuring the lasting success of your dental implant.
Regular Dental Check-ups & Professional Cleanings
Consistent professional care is vital for the longevity of your dental implant. Schedule regular dental check-ups – typically every six months – allowing your dentist to monitor the implant’s stability and surrounding tissues. These appointments enable early detection of potential issues, preventing minor problems from escalating into significant complications.
Professional cleanings remove hardened plaque (tartar) that brushing and flossing can’t eliminate. This tartar buildup can lead to peri-implantitis, an inflammation around the implant that can jeopardize its success. Your dental hygienist will use specialized instruments to carefully clean around the implant without damaging it.
During these visits, your dentist will also assess your bite to ensure it’s not placing undue stress on the implant. Don’t hesitate to discuss any concerns or changes you’ve noticed in your mouth. Proactive dental care is a key investment in the lasting health and functionality of your dental implant.

Avoiding Habits That Can Damage Implants
Protecting your investment requires avoiding certain habits that can compromise your dental implant’s integrity. Smoking significantly increases the risk of implant failure due to impaired healing and reduced blood flow. It’s strongly advised to quit smoking before and after implant placement.
Using your teeth as tools – opening packages, biting nails, or chewing on hard objects like pens – can exert excessive force, potentially damaging the implant or surrounding teeth. Similarly, bruxism (teeth grinding) can place undue stress on the implant; a nightguard can mitigate this risk.
Hard and sticky foods, especially in the initial healing phases, should be avoided. While implants are strong, they aren’t immune to damage. Proper oral hygiene, combined with avoiding these detrimental habits, will ensure the long-term success and stability of your dental implant, allowing you to enjoy a confident smile for years to come.
Recognizing and Addressing Late Complications
Long-term implant success relies on vigilance, as complications can arise even years after placement. Peri-implantitis, an inflammatory condition affecting the tissues around the implant, is a significant concern. Symptoms include redness, swelling, bleeding, and even implant loosening – requiring prompt professional intervention.
Mechanical issues, such as screw loosening or component fractures, can occur over time due to wear and tear or excessive force. Changes in bite or the development of cracks in the restoration can also signal problems. Regular dental check-ups are crucial for early detection.
If you experience any unusual sensations, pain, or changes around your implant, contact your dentist immediately. Early diagnosis and treatment are key to preventing further damage and preserving your dental implant; Ignoring these signs can lead to implant failure and necessitate more complex and costly procedures.
